What is Nutritional Pharmacology?
Back in the 1980s, a scientist at Syntex Research in Palo Alto, California by the name of Gene A. Spiller defined nutritional pharmacology as:
“The study of substances found in foods that might have a desired pharmacological effect when fed in higher concentrations and/or in purified or chemically modified form even though these compounds might not be nutrients per se.”
In his definition, Mr. Spiller was referring to the fact that, when taken in larger amounts than normally present in our diets, certain food components exercise an effect that cannot be considered either nutritional or physiological. Instead, the effect is classified as pharmacological.
A few substances that Mr. Spiller considered to be derived from nutritional pharmacology research include:
- Concentrated fiber polymers as bulking agents (Psyllium seed, gums, etc.)
- Modified retinoids (Vitamin A-related compounds) in the prevention of carcinogenesis
- Modified Vitamin D for certain bone diseases
- Sterols for the control of cholesterol absorption
- Choline in brain disorders associated with deficient central cholinergic tone
- Trisaccharides in hepaticcoma
- Gums in adult onset diabetes
Dr. Spiller’s initial findings and hypothesis would eventually pave the way for a plethora of research and studies regarding the use of minerals, vitamins, botanicals, and phytochemicals as nutritional supplements that affect specific functions or diseases (The American Journal of Clinical Nutrition, 1980).
Nutritional Pharmacology at Work
The topic of nutritional pharmacology emerged in the 1990s in a series of studies conducted in relation to burn victims, HIV, and inflammation, with promising results.
Burn Victims & Amino Acids
Burn victims typically experience painful and extremely harmful pathophysiological alterations including extensive nitrogen loss, malnutrition, an increased metabolic rate, and immunologic deficiency. As a result, these alterations predispose burn victims to more frequent infection, decreased chance of wound healing, longer hospital stays, and higher death rates.
However, with proper nutritional support, these effects can be prevented or decreased. Studies have shown that, if administered soon after injury in quantities two to seven times the normal amount, dietary components such as glutamine, arginine, and (n-3) fatty acids can have beneficial pharmacological effects on the alterations burn victims typically experience (The Journal of Nutrition, 1998).
Flavonoids & HIV
An article published in the American Journal of Clinical Nutrition titled “Nutrition & Pharmacology: General Principles and Implications for HIV”, Daniel J. Raiten sheds light on the interaction between food, nutrition, and drug metabolism in the prevention, care, and treatment of HIV.
Raiten defines nutrition as “the sum total of the processes involved in the taking in and use of food substances through which growth, repair, and maintenance of activities of the body as a whole or in any of its parts are accomplished.” He establishes the primary processes of nutrition as ingestion, digestion, absorption, metabolism, functional use of dependent systems, and excretion and claims that each of these processes are integral to how the body takes in and uses nutrients and other food components.
One group of substances that was of particular interest to those studying nutritional pharmacology in relation to HIV was the flavonoid group. According to Raiten, “flavonoids are a group of substances that occur naturally in fruit (including cocoa), vegetables, beverages (tea, wine), and many dietary supplements (ginkgo biloba) or herbal remedies.”
Research about flavonoids has shown that this group has beneficial effects on a variety of different health conditions, including HIV. Flavonoids significantly affect the activity of CYP – the most abundant isoform of the cytochrome system in the human liver, which is responsible for the metabolism of approximately 60% of HIV-related drugs (The American Journal of Clinical Nutrition, 2011).
Omega-3’s as Anti-Inflammatories
Many studies have been conducted assessing the benefits of supplementing fish oil in diets of humans suffering from inflammatory and autoimmune disorders such as Crohn’s disease and rheumatoid arthritis. Fish oil is high in omega-3 fatty acids, which have shown to be successful in the management of inflammatory and autoimmune diseases in both humans and animals due to their anti-inflammatory properties.
According to a study conducted by the Center for Genetics in Washington DC, fish oil has revealed to have a significant benefit in treating ulcerative colitis, Crohn’s disease, psoriasis, arthritis, multiple sclerosis, and migraine headaches (US National Library of Medicine, 2002).
Hemp as a Therapeutic Agent
Rather than treating each system with a dedicated nutrient or substance group, studies point to the possibility that there are groups of plant compounds that have the ability to impact many ailments related to almost every body system: hemp compounds are a prime example.
Throughout history, hemp has been used as a therapy for issues from leprosy to earaches to the common headache. However, it took thousands of years before anyone found an answer to the question: how could one plant treat so many diverse ailments? The answer lies in a hitherto unknown system in the body that affects how almost every other system works: the ECS.
The ECS
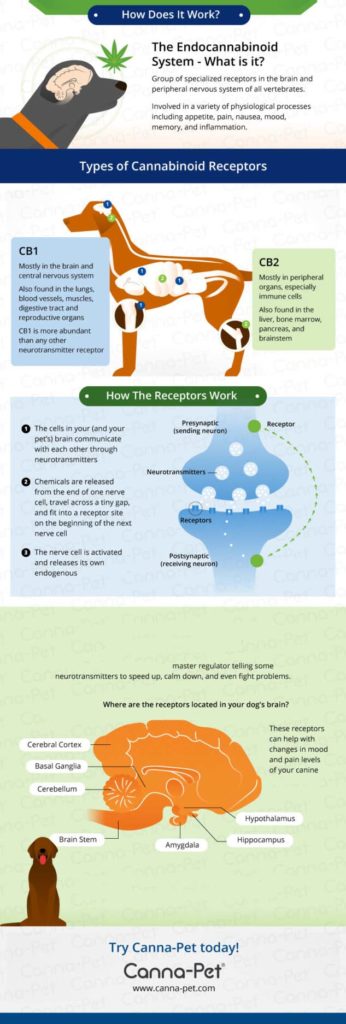
The ECS consists of a group of specialized receptors in the brain and peripheral nervous system of all vertebrates and is involved in a variety of physiological processes including:
- Appetite
- Pain sensation
- Nausea
- Mood
- Memory
- Inflammation
In 1964, Dr. Ralph Mechoulam identified THC as the chemical in marijuana that was responsible for making people feel high – the first “hemp compound.” But that discovery didn’t fully explain how hemp quelled nausea or seizures and lessened pain. Experiments showed that THC didn’t work with the endorphin system or any other known body system. It left many scientists scratching their heads: where were receptor sites in the brain?
…As it turns out, the answer is just about everywhere! In the late 1980s, scientists found receptor sites all over the brain that reacted to THC. They discovered that these receptors, called CB1, were abundant in the brain.
Then scientists discovered a second type of receptor, which they called CB2. While CB1 receptors are mostly in the brain and central nervous system, CB2 receptors are mostly in the peripheral cells, especially immune system cells.
CB1 receptors can also be found in the lungs, blood vessels, muscles, digestive tract, and reproductive organs while CB2 receptors can be found in the liver, bone marrow, pancreas, and brainstem. Basically, these receptors are found through our, and our pet’s, bodies and brains!
How Does the ECS Work?
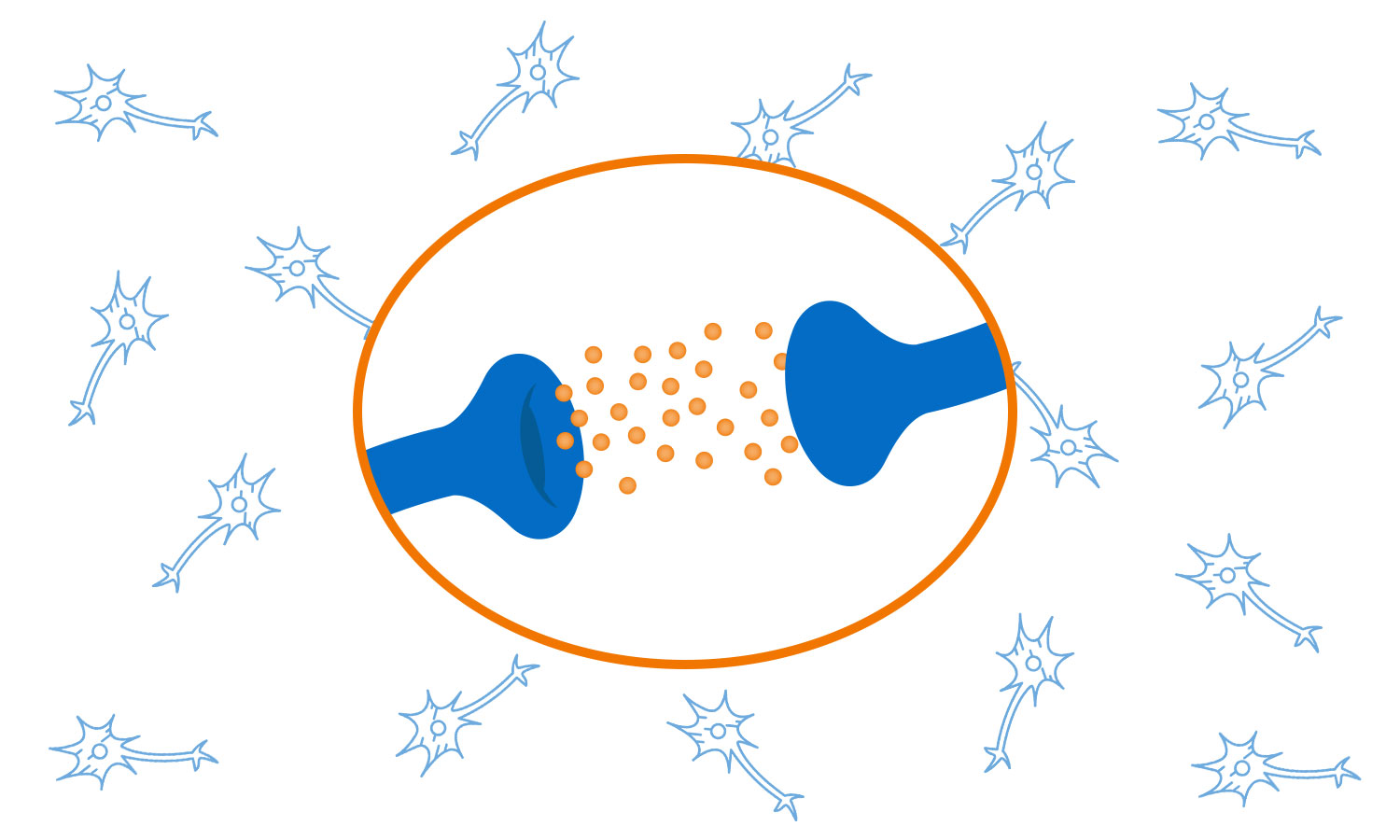
The cells in your brain and nervous system communicate with each other by means of various types of chemicals called neurotransmitters. Specific chemicals are released from the end of one nerve cell, travel across a tiny gap, and fit into a receptor site on the beginning of the next nerve cell.
Once the next nerve cell is activated, that cell releases its own endogenous compounds, which travel backward across the same gap to the nerve cell that released the neurotransmitter, attach to a receptor on that nerve cell, and tell the nerve cell to cut down on releasing the neurotransmitter. It acts sort of like a thermostat.
The body produces its own neurotransmitters and its own endogenous compounds. Each type of neurotransmitter and compound fit only in certain receptors because the receptor is shaped so it only accepts certain shaped chemicals, like a lock and key.
And as it turns out, our bodies naturally produce our own endogenous compounds that interact with the ECS. Because the phytochemicals found in hemp closely mimic the body’s endogenous compounds, they elicit the same response from receptors as the body’s endogenous compounds would.
And this phenomenon isn’t specific to humans. The ECS system was found in primitive sponges 600 million years ago as well as all mammals, birds, reptiles, and fish today. As a result of this high frequency, it was hypothesized in 2005 that the evolution of receptors was directly linked to the evolution of multi-cellular animals. Clearly the ECS system serves a vital function in our survival and evolution.
After further studies, scientists discovered that these compounds modulate every other neurotransmitter in the body. Acting as a master regulator, these compounds tell other neurotransmitters to speed up, calm down, fight problems, or restore the body back to its normal state.
When we have an infection, ECS signals tell the immune system to fight it, and when the invader is destroyed, to back down. These compounds perform this function in numerous body systems, working to maintain the body’s homeostasis.
Hemp Components Beyond THC
THC is far from the only compound identified in hemp – since the 1980s therapeutic properties have been attributed to numerous compounds. There are dozens of other components found in the hemp plant that have beneficial properties, beyond those of the amino acids, proteins, and omega-3s found in the plant. These include terpenes, and flavonoids.
Hemp Compounds
Recently, new compounds beyond THC have earned attention and generated excitement among the medical community. Unlike THC, hemp lacks psychoactive effects and has much lower toxicity limits. Not only do non-psychoactive hemp compounds have much higher safety levels than THC, but it also appears that many of the health benefits that “medical hemp” has been getting credit for are actually the work of industrial hemp and other non-psychoactive compounds beyond THC.
A 2009 article reviewing the therapeutic actions of non-psychoactive compounds cited numerous studies correlating hemp (specifically, other than THC) to numerous therapeutic benefits:
- Antianxiety
- Antipsychotic
- Antiepileptic
- Neuroprotective
- Blood vessel relaxant
- Antispasmodic
- Anticancer
- Antinausea
- Antidiabetic
- Analgesic
- Antibacterial
- Anti-inflammatory
- Immunosuppressive
- Bone Stimulant
Whole-plant hemp extracts exclusively used by Canna-Pet® contain dozens of activated compounds.
Terpenes
Terpenes are organic compounds usually known for their strong fragrance and flavor. While terpenes are prevalent in hemp, they are also found in thousands of other plants besides hemp.
Terpenes are FDA-approved food additives, common in both human and animal diets, that can interact with compounds in beneficial ways. For example, the terpene myrcene aids in allowing compounds to cross the blood-brain barrier and is associated with antidepressant, anti-inflammatory, anti-microbial, anticarcinogen, and antioxidant properties. In addition, the terpene limonene is known to stimulate the immune system and reduce gastroesophageal reflux.
Flavonoids
In addition to terpenes, hemp plants also contain flavonoids, plant metabolites known for their antioxidant and anti-inflammatory benefits. Quercetin is a type of flavonoid found in plant foods, including leafy greens, tomatoes, berries, and broccoli. It is also found in hemp. Quercetin is now largely utilized as a nutritional supplement to combat diabetes, obesity, circulatory dysfunction, inflammation, and mood disorders.
Another flavonoid called apigenin is found in fruits and vegetables such as parsley, onions, oranges, tea, wheat sprouts, and hemp has been shown to possess remarkable anti-inflammatory, antioxidant, and anti-carcinogenic properties.
ECS Deficiency
It is apparent that hemp compounds are an essential part of lifelong nutrition. But what happens when a person or animal is deficient in normal levels?
It’s widely known that deficiencies in a variety of normal body chemicals are often found and can lead to suboptimal health or full-blown disease. When deficiencies of nutrients are discovered, drugs or supplements are typically used to pick up the slack. In the case of ECS deficiency, we are fortunate that we can replace them with plant-derived compounds.
Could it be that people and pets who are susceptible to cancer (or anxiety or glaucoma or seizures) are hemp compound deficient?
In 2003, and again in 2014, researchers found that “underlying ECS deficiencies indeed play a role in migraine, fibromyalgia, irritable bowel syndrome, and a growing list of other medical conditions” (Neuroendocrinology Letters, 2014).
Dr. Narda Robinson, of Colorado State University, in her article Hemp for Intractible Epilepsy (Veterinary Practice News, June 2014) associates ECS deficiency with seizures, referencing a study in Experimental Neurology.
Hemp Compounds & Wellness
Activated Hemp Compounds are becoming vital tools in the fight against disease – but even more important is their value in maintaining health. This is especially true for middle-aged or senior pets. Modern advances in canine nutrition, medication, and therapies mean dogs are now living longer than ever. However, that often means that they are living longer with health issues.
Hemp nutrition may prevent and combat common complaints of aging, including diminution of mental capacities, anxiety, lack of appetite, and inflammation and pain associated with arthritis. But beyond that, hemp compounds may simply make pets feel better, improving their comfort, mood, activity and appetite, so they feel and act like a younger version of themselves – for longer!
Therapeutic Hemp Products for Your Pet
Several companies now offer hemp products for pets. The pioneer in the field of safe, legal hemp products for pets is Canna-Pet®. Canna-Pet products contain over two dozen compounds, terpenes, and flavonoids – through their exclusive use of whole-plant extracts.
Canna-Pet® is the only hemp brand for pets recognized by the United States Patent and Trademark Office, and that is why customers should look for the ® Registered Mark on our goods.
Our products and our results are unique.
When you are purchasing hemp products for your pet, remember that a safe and effective hemp product should:
- Use organic, quality screened, toxin-free hemp
- Be produced using whole plant CO2 extracts
- Be screened for hemp levels and toxins
- Provide an abundance of activated hemp compounds and terpenes, not just hemp
- Effectively deliver those compounds to your pet’s ECS with high bioavailability
- Come with a money-back satisfaction guarantee